 Previous literature has demonstrated that for general infections, patients with β-lactam allergies are more likely to receive suboptimal therapy, experience clinical failure, have an increased hospital length of stay, develop drug resistant organisms, and have higher in-hospital mortality. Most literature suggests that 99% of these patients do not have a true allergy and can safely receive β-lactam antibiotics. Additionally, true IgE-mediated allergies are relatively rare and electronic medical record descriptions of β-lactam allergies are often lacking or incomplete. Common clinical practice is to avoid other β-lactam classes, including cephalosporins, in patients with a labeled β-lactam allergy. While only 1–3% of the population report a cephalosporin allergy, patient-reported or poorly described β-lactam allergies represent a barrier to receiving cephalosporin therapy due to misconceptions related to cross-reactivity. 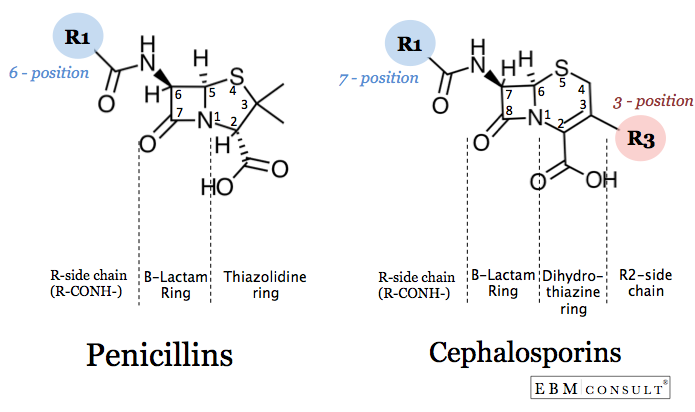
The purpose of this review is to provide an overview of the role of cephalosporins in clinical practice, and to highlight the incidence of, risk factors for, and cross-reactivity of cephalosporins with other antibiotics.Ĭephalosporins are a commonly prescribed class of antibiotics in inpatient and community settings due to their clinical utility in a number of infectious disease states. Clinicians should consider the low likelihood of true cephalosporin allergy when clinically indicated. Cephalosporin cross-reactivity potential is related to the structural R1 side chain, and clinicians should be cognizant of R1 side chain similarities when prescribing alternate β-lactams in allergic individuals or when new cephalosporins are brought to market. Risk factors for cephalosporin allergies are broad and include female sex, advanced age, and a history of another antibiotic or penicillin allergy however, cephalosporins are readily tolerated even among individuals with true immediate-type allergies to penicillins. The misdiagnosis of β-lactam allergies and misunderstanding of cross-reactivity among β-lactams, including within the cephalosporin class, often leads to use of broader spectrum antibiotics with poor safety and efficacy profiles and represents a serious obstacle for antimicrobial stewardship. However, clinicians may avoid the use of cephalosporins in patients with reported penicillin allergies despite the low potential for cross-reactivity. Thus, our data indicate that cephalosporins can be considered for patients with penicillin allergy.Cephalosporins are among the most commonly prescribed antibiotic classes due to their wide clinical utility and general tolerability, with approximately 1–3% of the population reporting a cephalosporin allergy. Cross-reactivity is not an adequate explanation for this increased risk, and the risk of anaphylaxis is very low. Patients with allergic-like events after penicillin had a markedly increased risk of events after either subsequent cephalosporins or sulfonamide antibiotics. The unadjusted risk ratio for sulfonamide antibiotic, rather than cephalosporin after penicillin allergic-like events was 7.2 (confidence interval 3.8-13.5). The absolute risk of anaphylaxis after a cephalosporin was less than 0.001%. Among patients receiving a penicillin followed by a cephalosporin, the unadjusted risk ratio of an allergic-like event for those who had a prior event, compared with those who had no such prior event, narrowly defined, was 10.1 (confidence interval 7.4-13.8). 
Comparison was made with a population of patients receiving a prescription for a penicillin followed by a prescription for a sulfonamide antibiotic.Ī total of 3,375,162 patients received a penicillin 506,679 (15%) received a subsequent cephalosporin. 
Allergic events were defined by 2 sets of codes: 1 more restrictive, 1 more inclusive. 
We selected all patients receiving a prescription for penicillin followed by a prescription for a cephalosporin and identified allergic-like events within 30 days after each prescription. We conducted a retrospective cohort study using the United Kingdom General Practice Research Database. We sought to determine the risk of an allergic reaction to a cephalosporin exposure in those with prior penicillin reactions. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
